Psoriasis
What is Psoriasis?
About 3% of people around the world suffer from psoriasis, a skin disorder characterized by inflammation, itching, pus-filled blisters, excessively dry skin, and silvery and flaky plaques that appear on one’s lower back, elbows, knees, groin and scalp (International Federation of Psoriasis Associations, University of Maryland Medical Center). As the severity of psoriasis increases, so does the likelihood of developing other comorbities like a short-lifer span and cardiovascular diseases(International Federation of Psoriasis Associations). Those who suffer from both psoriasis and psoriatic arthritis are also more likely to develop Crohn’s Disease, certain cancers, depression, obesity, metabolic syndrome and diabetes, among other conditions (National Psoriasis Foundation).
The medical community has yet to uncover the exact causes of psoriasis. However, it is known that psoriasis can develop when T-cells attack skin cells. Newer skin cells in turn move to the outer layers of the skin and proliferate so rapidly that they begin to pile upon one another, leading to psoriasis’ characteristic plaques (University of Maryland Medical Center). Growing research suggests that psoriasis may be due in part to inheritable genes that put one at a predisposition to develop psoriasis. Research has also suggested that stress, skin injuries, and certain medications may play a role in psoriasis’ development, though more research is needed to understand this potential relationship (National Psoriasis Foundation) Causes may also include excessive alcohol consumption or smoking, obesity, and exposure to cold weather, though these possible triggers are under investigation(University of Maryland Medical Center).
How Often Should I Exfoliate Skin with Psoriasis?

What Ingredients are Best for Psoriasis?
Exfoliating dry skin, especially plaque-laden psoriatic skin, can be very tricky. Those with psoriasis and similar conditions should limit exfoliation to once a week or less, unless given different instructions from their dermatologists (American Academy of Dermatology). Too frequent exfoliation can further inflame the skin and zap it of whatever precious moisture it may be left in the skin..
Capsaicin
Capsaicin is the chemical compound that gives peppers their characteristic spice. Of course, applying a spicy compound onto already inflamed skin sounds like a terrible idea in theory, but don’t be so quick to discount capsaicin; studies have repeatedly demonstrated its aptitude in treating inflammation, psoriasis, and general pain. Topically-applied capsaicin significantly improved psoriasis vulgaris-induced erythema and scaling, in addition to the overall appearance of psoriatic skin (Journal of the American Academy of Dermatology) Capsaicin has also proven itself to be of benefit in treating the overall severity of pruritic psoriasis, a condition characterized by excessively itchy psoriatic plaques and patches (Journal of the American Academy of Dermatology). When applied topically, capsaicin has also improved soft tissue pain such as back pain and arthritis (Phytotherapy Research, Clinical Therapy) . Given capsaicin’s analgesic and anti-pruritic properties, it is reasonable to believe that capsaicin will be of benefit in treating inflamed and pained psoriatic lesions, though research is needed to confirm this relationship.

Coal tar
Coal tar was once a common psoriasis treatment, but this ingredient’s propensities for staining clothing, its foul odor, and general messiness have made it a less desirable treatment to some. Nevertheless, the skin care industry is in the midst of altering coal tar in such a way that it is more appealing to consumers, because this treatment really is quite effective in soothing psoriasis, atopic dermatitis, and several other dry skin conditions (Journal of the American Academy of Dermatology, Journal of Drugs in Dermatology) Coal tar is both an antibacterial and antipruritic (anti-itch) agent that can inhibt deregulated epidermal proliferation (Dermatology). But what does that mean for us psoriasis sufferers? By inhibiting regular epidermal proliferation, coal tar can assist in regulating the excessive cell growth that can contribute to psoriasis’ characterize plaques.
Jojoba Oil
What dry skin treatment would be complete without jojoba oil? Jojoba oil closely mimics skin’s natural oils, and the fatty acids within jojoba oils pair beautifully with our skin’s naturally-produced sebum. Even better, jojoba has demonstrated an aptitude to serve as an antibacterial, anti-inflammatory, analgesic and antioxidant agent, among numerous other roles.
Moisture
(Skin and Allergy News, European Scientific Journal, Pharmacology Research). Even better, jojoba oil is a penetration enhancer that assists other beneficial ingredients to work their magic in the deeper layers of skin (Journal of Cosmetic Science, Journal of the American Oil Chemists’ Society).
Tazarotene
Derived from Vitamin A, tazarotene is a commonly-prescribed topical treatment for mild to moderate instances psoriasis. Tazarotene’s primary function is to inhibit the accelerated cell growth that causes psoriatic lesions (International Federation of Psoriatic Associations) . In research published in the Journal of the American Academy of Dermatology, tazarotene was applied to psoriatic skin once a day for 12 weeks. After the trial period, the tazarotene was found to improve the overall appearance of psoriatic skin, especially plaque elevation and skin scaling. Similarly, researched published in the journal Clinical Therapy found that topically-applied tazarotene combined with topical mometasone furoate (a corticosteroid) improved scaling, erythema, and plaque height and reduced the amount of body surface area covered in lesions.
Salicylic Acid
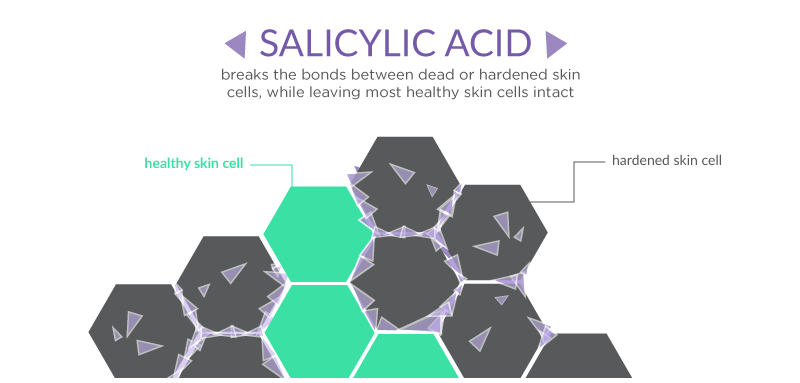
If we could, we would proclaim our love of salicylic acid from the rooftops. Salicylic acid is a beta hdyroxy acid (BHA) that is thought to be the most powerful keratolytic agent in dermatology today(Clinics in Dermatology). This BHA works by breaking down the cellular bonds between hardened skin cells, so that they may be more easily sloughed away (Archives of Dermatological Research) Not only does this allow your healthy skin to shine through, but it also loosens up scaly lesions so that other medications can penetrate more deeply into the skin, according to the International Federation of Psoriatic Associations . Need some more convincing that salicylic acid is a great ingredient? Check out our article, 5 Things That You Never Knew about Salicylic Acid Exfoliation.
Colloidal Oatmeal
The Journal of Drugs in Dermatology notes that colloidal oatmeal has often been employed to try dry skin conditions like atopic dermatitis and psoriasis. It is believed that colloidal oatmeal’s anti-inflammatory and antioxidant properties are what make it such a soothing topical treatment. In fact, a separate study from the Journal of Drugs in Dermatology found that colloidal oatmeal’s anti-inflammatory properties were likely responsible for treating roughness, scaling, itching, and dryness in participants who had moderate to severe dry skin on their legs.
Which ViaBuff Puff Should I Use?

While the thought of rubbing an abrasive exfoliating puff on psoriatic skin is about as appealing as hearing nails on a chalkboard, think again; exfoliation is necessary so as to remove dried and flaky skin, as well as to allow other topical treatments to penetrate more deeply into the skin. We designed the ViaBuff Level 1 Exfoliating Puff to be gentle on even the most sensitive skin while kicking dried, dead skin to the curb. Each of our puffs limit water retention, which in turn limits the rate and probability of bacterial colonization on the puffs. Additionally, our puffs last for about to 90 days (though our customers report several months!), which is about three times longer than most standard puffs and loofahs. Even better, we offer the Level 1 Puff as both a Body Puff and Facial Puff, and offer a ViaBuff Handle so that you can reach those hard-to-exfoliate places.



